
CASE NOTES
Bacterial meningitis in a ram
Rahul Shankar - District Veterinarian (DV), Young and Erika Bunker - Veterinary Pathologist, EMAI
Posted Flock & Herd August 2017
Introduction
Causes of meningitis, encephalitis and encephalomyelitis include viruses, bacteria, fungi, protozoa, rickettsia, parasites and chemical agents. In ruminants, bacterial meningitis is most commonly seen and has been described in both neonates and adult animals.
This case report describes an animal exhibiting severe neurological symptoms and was eligible for the National Transmissible Spongiform Encephalopathy Program (NTSEP). The NTSEP underpins our market access with our trading partners. Scrapie is not present in Australia or in New Zealand, yet prevalent in other developed nations throughout the world. Through vigilant surveillance activities conducted by District Veterinarians and Veterinary Officers throughout Australia we are able to prove our freedom from this disease by selecting suitable candidates for TSE rule-outs. Neurological conditions offer prime candidates (assuming they also fit the age parameters) for TSE exclusions and veterinarians are encouraged to submit samples to aid the NTSEP.
Case report
A producer east of Young reported unusual symptoms in one of his young White Suffolk polled rams (approx. 2-3 years old). The weather in Young to date had been fairly dry with many producers supplementary feeding stock to get them ready for joining. Recent rains had broken the dry spell and paddocks were starting to show growth. The ram mob had been in a short, dry feed paddock with no access to supplements.
The affected ram was described as having seizures for periods of up to 30-45 seconds, with the animal undergoing 2-3 successive fits within approximately 15 seconds of each other. Once the animal rose and was able to ambulate, the owner described the affected animal to have uncoordinated movements - acting 'drunk'. No wounds were observed around head or poll of the ram. There were no signs of trauma to the ear or any other part of the body. The owner did not notice any signs of a head tilt or eyelid drooping. Unfortunately a field visit could not be conducted to examine the animal ante-mortem (call occurred on a weekend and DV was not in the area), however the owner was advised to try a response to therapy in the interim. The owner removed the ram from the ram paddock and isolated this individual with access to hay andad lib water. Vitamin B1 was injected (approx. 1ml/10kg) IM three times over a 24 hour period.
Differential diagnoses at this stage included: polioencephalomalacia, trauma leading to an infection, and otitis media.
The next day the owner reported to the DV that the animal was showing signs of recovery with the animal able to stand, and even charged at the owner on one occasion. The owner attempted to hand feed grain to the affected ram, which it accepted but was followed by the animal deteriorating rapidly by displaying several grand mal seizures in a period of 3 hours. The animal was able to recover in between seizures. During the course of the day the owner noted that the ram was blind in one eye (owner could approach the ram from one side over the other without the ram noticing him) and was no longer able to rise without assistance. The owner also noticed that the poll of the ram had brownish coloured exudate along with whitish exudate emanating from it, however he remarked that he had not noticed this on the ram earlier and this may have well occurred during one of his fits while he was thrashing violently on the ground. The ram subsequently fell into lateral recumbency and within 20 minutes died.
Post-mortem and histopathology
A property visit was conducted to examine the ram to gain an understanding of what underlying cause this ram had died from.
The ram had no external injuries to its torso but had dried exudate coming from its left poll. Both ears showed no signs of trauma or inflammation. An exploration of each ear canal revealed no abnormalities either. A post-mortem examination of the abdominal and thoracic cavity revealed no abnormalities in any of the body organs examined.
Upon opening the cranial cavity the right cerebral hemisphere was covered in a creamy greenish-yellowish exudate on the lateral aspect that extended into and stained the associated side of the cranial cavity. A morphologic diagnosis of acute, severe, diffuse suppurative meningitis was made and relevant diagnostic samples in the form of fixed brain and a sterile swab were taken for analysis. As the animal fit multiple criteria for a TSE exclusion, this case was also used for the purposes of the NTSEP incentive program.
Histology confirmed this diagnosis. There was a severe multifocal acute to subacute suppurative meningitis with focal thrombosis and vascular necrosis. The meninges were severely expanded by accumulations of degenerate neutrophils, loose infiltrates of mixed inflammatory cells, oedema, congestion and haemorrhage; bacterial colonies were noted. One meningeal artery contained a fibrin thrombus, and there was necrosis of the vessel wall. Haemorrhage and inflammation were extending into the subjacent cortical grey matter which also showed oedema with faded eosinophilic neurones.
The culture returned a profuse dominant growth of Truperella pyogenes (T.pyogenes).
The animal was also TSE negative on histopathology.
Video 1 and Video 2. Grand-mal seizures involving the affected ram
Gross pathology Images

Image 1: Affected brain and cranial cavity
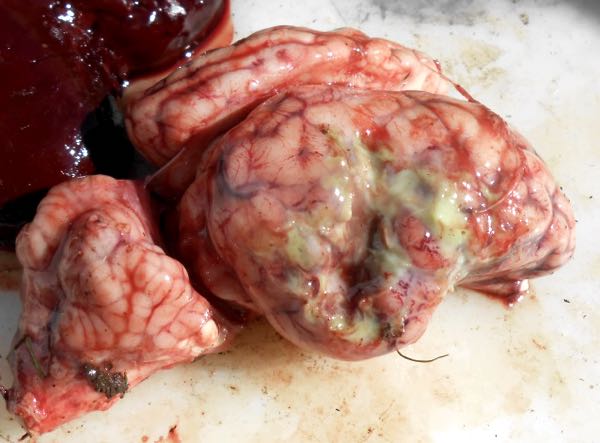
Image 2: Close up of the affected portion of the brain
Histopathology:

Image 3: Cerebral meningitis with oedema.

Image 4: Thrombosed and necrotic vessel in the meninges and massive destruction with haemorrhage in the underlying cerebrocortical grey matter
Discussion
The pathogenesis of the suppurative meningitis in this particular case remains unknown. Abscesses in the brain commonly originate from haematogenous spread, direct spread from injury to the cranium or via the nasopharynx1. Infectious agents are able to attack the CNS via retrograde infection via peripheral nerves, direct penetrating injuries, extension of adjacent suppurative lesions or by way of systemic circulation1.
Pituitary abscess syndrome is well described in the literature and could have been attributed to this particular case. Pituitary abscesses occur spontaneously in ruminants with the causative agent being T.pyogenes in cattle2. The occurrence of pituitary abscesses is low (< 2% in outbreaks). Male animals, 2-5 years of age seem to be most susceptible, which has been attributed to the tendency of male animals to fight one another and head injuries resulting. Neurologic signs include depression, dysphagia, dropped jaw, blindness and a lack of a pupillary light reflex. In cattle, the use of a nose ring appears to be a predisposition to this cause, leading to sepsis1. There are 2 ways a pituitary abscess could occur: either by haematogenous spread to the rete mirabile (which surrounds the pituitary gland) or via the cavernous sinus3.
Haematogenous infection is common in neonatal septicemia arising from failure of passive transfer. Lambs 3-8 months of age are more often diagnosed with brain abscessation attributed to the mild docking / castration lesion caused by castrator rings4. The lesion more often affects one cerebral hemisphere and the affected animals present with contralateral blindness, normal pupillary light reflexes and contralateral proprioceptive deficits4.
It is important to note that many cases of brain abscess are clinically similar to otitis media, however in otitis media cases there is frequently rotation of the head, a commonly associated facial paralysis and an absence of signs of cerebral depression1. The only specific disease where abscesses are known to occur is Listeriosis where the lesion is often confined to the medulla oblongata and clinical signs would normally include circling and unilateral facial paralysis. Fungal infections such as Cryptocooccus and parasitic infections such as Toxoplasmosis are uncommon, but occasional cases may also see associated lesions1.
Case-fatality rates in affected animals with bacterial meningitis is high, owing to the late stage diagnosis of cases. Antibiotics, anti-inflammatory drugs and anti-seizure medication have a role in animals that are of worth to their owners. Antibiotic selection should be based on an evaluation of CSF by culture and sensitivity. A 3rd generation Cephalosporin given IV at a rate of 1-5 mg/kg, once to three times daily has been shown to be beneficial. Combination antibiotics have also been used in some cases. Seizures can be controlled with diazepam at a rate of 0.01mg/kg to 0.2 mg/kg every 30 minutes2. Such intensive care for animals, coupled with the associated veterinary costs would make such recommendations not feasible for many farmers, and humane euthanasia of affected animals should be considered in any case deemed necessary.
An interesting question to rise is whether the incidence of meningitis, encephalitis or myeloencephalitis occurs more in polled animals as compared to non-polled animals? A literature search did not reveal much in terms of a comparison, and it would be interesting to collate data to see whether such an association exists.
References
- Radostits O, Done S. Veterinary medicine. 1st ed. Saunders Elsevier, Edinburgh, 2007
- Fecteau George L. Bacterial meningitis and encephalitis in ruminants. Veterinary Clinics of North America: Food Animal Practice 2004; 20:363-377
- Morin D. Brainstem and cranial nerve abnormalities: listeriosis, otitis media/interna, and pituitary abscess syndrome. Veterinary Clinics of North America: Food Animal Practice 2004; 20:243-273
- Aitken I. Diseases of sheep. 1st ed. Blackwell Pub., Oxford, 2007

